Suggested CitationGidwani R, Hong J, Murrell S. Fee Basis Data: A Guide for Researchers. Health Economics Resource Center, VA Palo Alto Health Care System, U.S. Department of Veterans Affairs. November 2015.
DisclaimersAs of April 2019, this guidebook is no longer being updated. For current information on Community Care data, please visit the page VA Community Care Data.
All tables mentioned in the Fee Basis guidebook are stored in an Excel file. Download the tables here.
Many URLs are not live because they are VA intranet only. Researchers with VA intranet access can access these sites by copying and pasting the URLs into their browser.
For a list of VA acronyms, please visit the VA Acronym Lookup on the VA intranet at http://vaww.va.gov/Acronyms/fulllist.cfm.
1. Introduction
The Department of Veterans Affairs (VA) often pays providers in the community to provide care to Veterans when it is unable to provide such care itself (e.g., due to a lack of resources or delays in providing care), or when it is infeasible to do so (e.g., emergency care). Such care is called Non-VA Medical Care, or Fee Basis care.
VA can make payments to non-VA health care providers under many arrangements. As noted above, non-VA care may be authorized under the Non-VA Medical Care program when VA cannot offer needed care. In addition, VA may place a Veteran in a private or state-run nursing home when a bed in a VA nursing home is unavailable or if the nursing home is distant from the patient’s residence. VA can also pay for hospice care for Veterans when the VA facility is unable to provide the needed care; this happens frequently, as VA provides only inpatient-based hospice care and many Veterans may wish to receive hospice at home or in the community. Payment for these types of care falls under the Non-VA Medical Care program. Non-VA Medical Care consumes a significant portion of VA spending; indeed, contract costs (i.e., the cost of all things purchased from non-VA health care providers) accounted for approximately 11% of VA expenditures in fiscal year 2014.
Many veterans now have access to Non-VA medical care through the new Veterans Access, Choice, and Accountability Act (VACAA, or “Choice Act”). The Choice Act represents one of the largest shifts in the organization and financing of healthcare in the Department of Veterans Affairs (VA) in recent years. Passed in 2014 with bipartisan support in Congress, its purpose is to increase Veterans’ access to health care.1 The Choice Act allows Veterans to receive health care through non-VA providers in the community if they are unable to schedule an appointment at their local VA within 30 days or by a date determined by their provider (“wait-time goals”), if they reside over 40 miles from a VA facility, or if they face an unusual or excessive burden in travelling to a VA facility.2 Under the Choice Act, ten ($10) billion dollars has been allocated towards Non-VA Medical Care for eligible Veterans through 2017.1 The Fee Basis files contain data for care received through the Choice Act, but in this guide, we do not distinguish for care provided under the Non-VA Medical Care program and that provided under the Choice Act. Persons interested in studying care provided under the Choice Act may wish to explore the VACAA tables or the FBCS tables at VA Corporate Data Warehouse (CDW).
Fee Basis data will be most useful for studying conditions where contract care is common, such as home-based care and nursing care, and for determining typical non-VA charges for health care services (both charges and payments are reported) and comparing those to VA costs. There is also a host of non-emergency surgery provided through Fee Basis mechanisms that may be of interest to researchers.
This guidebook is intended to help researchers understand and use the National Fee Basis files, which come in both SQL and SAS formats. This guidebook describes characteristics of Fee Basis care data such as contents and missingness, and makes recommendations about its use for research purposes. Chapter 1 presents an overview of Fee Basis data in general; Chapter 2 presents an overview of the variables in the Fee Basis data; and Chapter 3 describes how SAS versus SQL forms of Fee Basis data differ. Chapter 4 offers detailed information SAS Fee Basis data; Chapter 5 provides detailed information about SQL Fee Basis data. Chapter 6 provides information about how to access the Fee Basis data, while Chapter 7 provides information about the rules governing Fee Basis care. Chapter 8 provides references for further information about the Fee Basis program and data.
1.1 Overview of Fee Basis data
Fee Basis data are housed in VA in both SAS dataset format and Microsoft SQL server tables (hereafter referred to as SQL data). Both the SAS and SQL Fee Basis are housed at VINCI; the SQL data is also found at the Corporate Data Warehouse (CDW). The CDW is a relational database organized into a collection of data domains implemented on the Microsoft SQL server in VINCI. At the time of writing, SAS data at CDW are available only to those persons with VA operations access. Researchers wishing to work with SAS Fee Basis data can access them at the Austin Information Technology Center (AITC). Of note, SQL and SAS data contain similar, but not exactly the same, information. We detail differences amongst the SAS and SQL Fee Basis data in the guidebook below. Summary Fee Basis expenditure data are also available through the VHA Support Services Center (VSSC) intranet site, further information about accessing these summary data can be found in Chapter 6.
Fee Basis data can be broadly categorized into 4 classes: inpatient care, outpatient care, pharmacy, and travel data. There is limited information on the providers associated with Fee Basis care. Fee Basis data files contain information regarding both the care the Veteran received and the reimbursement of the care. All Fee Basis care will be found in the Fee files. Some Fee Basis data will also appear in the non-VA medical SAS inpatient file (formerly called the Patient Treatment File). For the purpose of this guidebook, we focus on Fee Basis files only.
In both the SAS and the SQL data, there are usually multiple observations per patient encounter. This is true for both the inpatient and the outpatient data, albeit for different reasons. In the Fee Basis inpatient data, each record represents a separate claim; these separate claims must be aggregated to capture the totality of the inpatient stay. The inpatient data will also need to be linked to the ancillary data, or the data representing the professional services provided to a patient while in the hospital, in order to determine the total cost of the inpatient stay. In the outpatient data, each record represents a different procedure, as assessed through the Current Procedural Terminology (CPT) code. There may be multiple CPT codes associated with a single encounter. Therefore, on the outpatient side as well one must aggregate multiple records to get a full picture of the outpatient encounter.
The Fee Basis data contain a unique variable not found in the traditional VA inpatient and outpatient datasets: the Fee Purpose of Visit (FPOV) variable. This FPOV variable broadly categorizes the reason for the encounter, such as hospice or respite care. The FPOV variable can be found in both the SAS and SQL data.
1.2 How a Veteran accesses Non-VA care
The VA pays for both emergency and non-emergency care through Fee Basis mechanisms. Non-emergency care must be approved before the Veteran seeks care in the community.3 For traditional Non-VA care, a Veteran’s VA provider will submit a request at the local VA facility for Veteran care provided by Fee Basis. This care will be approved (or denied) by the local VA Fee Office; the Veteran is then free to seek non-VA care. Claims related to this care are considered “authorized” care. For care received under the Choice Act, Veterans will work with the third party administrators of the Choice program to find an eligible provider in their area.4
There is another category of Fee Basis care that is considered “unauthorized” care. If the Veteran received care in the community that was not pre-authorized, it is considered “unauthorized” by VA. Thus, unauthorized care is not unpaid care – it is simply not PRE-authorized care. Most, if not all, of this care should be emergency care. Unauthorized care can be of an inpatient or outpatient nature. For example, if the Veteran had an Emergency Department (ED) visit and then was admitted to the hospital, this would be considered inpatient care. If the Veteran went to the ED and was not admitted to the hospital, this would be considered outpatient care. Regardless of whether the care was pre-authorized or not, non-VA providers submit claims to VA if they wish to be reimbursed for care.
1.3 Data capture
While all non-VA providers must submit a claim to VA in order to be reimbursed for care, the claim filing deadline depends on the type of claim. Authorized care claims must be submitted within 6 years of the date of service, service-connected emergency care claims must be submitted within 2 years of the date of service, and non-service-connected emergency care claims must be submitted within 90 days of the date of service/discharge. More information about provider reimbursement can be found in the document Working with the Veterans Health Administration: A Guide for Providers (available on the VHA Office of Community Care website, on the Provider Resources page).5
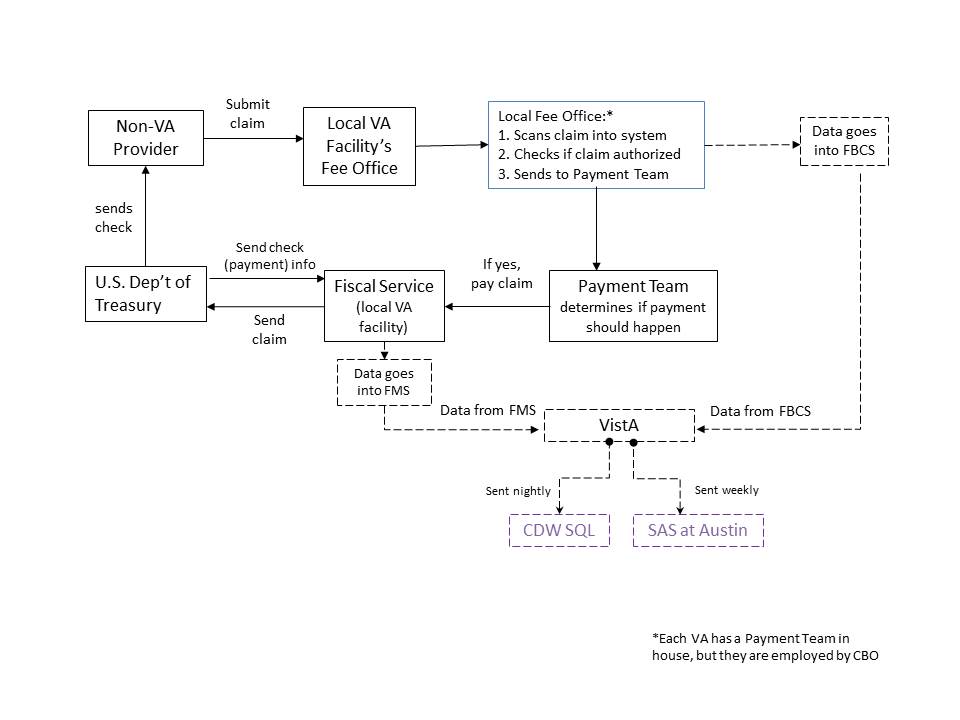
Each VA facility has a local Fee Office to which the non-VA provider submits a claim for reimbursement. The local VA facilities put claims through a claim scrubber that checks to see if the claim was authorized and evaluates any errors or inconsistencies in the data. All preauthorized claims are then processed through the Fee Basis Claims System (FBCS) at the local facility as well as sent to the payment team. The diagram below (Figure 1) displays how payment is processed and sent to the non-VA provider. The data regarding the clinical encounter as well as the charge and payment for that encounter are populated into the VA Health Information Systems and Technology Architecture (VistA). From there, it is sent weekly to AITC in SAS format and nightly to CDW in SQL format.
Of note, the FBCS was not in place nationwide prior to FY 2008. Before this time, data were entered by hand, and there was no easy way to tell whether the claim being entered was a duplicate one. Researchers should pay special attention to reducing duplicates in the pre-2008 data.
From 1998 to 2014, approximately 50% of claims were paid within 30 days of VA receiving the invoice, and 95% of claims are paid in 200 days or less. However, there are some outliers; some claims can take up to 8 years to process. The majority of claims, 99%, were processed within 2 years, with the exception of pharmacy data in FY 2004 and FY2008. Our review of the data suggests that pharmacy and ancillary claims take longer to process than inpatient or outpatient claims.
Figure 1. Non-VA Care Data Pathway
1.4 Transfers between VA and Fee Basis care
If the patient is transferred from a non-VA to a VA hospital, the non-VA component of this care will be captured through Fee Basis, while the VA component of this care will be in the VA inpatient datasets. Therefore, to get an understanding of the total cost of this care, one would have to link the Fee Basis data to VA utilization datasets. Researchers can look at the disposition variable as an indicator of transfer between VA and non-VA care. In SAS, this variable is called DISTYP, or disposition type, and is located in the Inpatient and Ancillary tables. In SQL, the fields containing these data can be found in the FeeDispositionCode and FeeDispositionName. Refer to Appendix C for a list of Fee Disposition Codes.
1.5 What’s new in this guidebook
The 2015 update to the Fee Basis Medical Care guidebook describes for the first time the SQL Fee Basis files, and contains a host of information about how SAS versus SQL Fee Basis files differ. This guide was published in October 2015; the same month the United States switched from ICD-9 to ICD-10. All information in this guidebook pertains to use of ICD-9 codes.
_________________________________________________________________
Notes and Recommendations
- Fee Basis data live in both SAS and SQL format. SAS and SQL data are very similar, but not exact copies of each other.
- Much Fee Basis care is pre-authorized prior to the Veteran obtaining care and is thus considered Authorized Care. Unauthorized Care is that which was not pre-authorized but was still reimbursed, such as emergency care.
_________________________________________________________________
2. General Overview of Fee Basis Data
In this chapter, we discuss general aspects of Fee Basis data. All persons working with these data should review this information before conducting any analyses. The discussion below pertains to both SAS and SQL data.
The Fee Basis files are stored in two formats: SAS and SQL. SQL Fee Basis data are stored in CDW in multiple individual tables. The SAS data are stored at AITC. SAS data are also available in CDW, but are currently limited to those VA employees with operational access. The SQL Fee Basis data at CDW and the SAS Fee Basis data at AITC are available for VA researchers following a standard approval process. Chapter 6 contains more information about how to access these data.
In SAS, data are stored in variables, observations and datasets. These correspond to fields, rows and tables in a relational database. Relational Database Management Systems (RDBMS) such as Microsoft SQL server have multiple hierarchies for storing data: a domain contains many schemas, which in turn contain many tables. Domains represent logically or conceptually related sets of data tables. Domains generally indicate the application in the VistA electronic health record system from which most of the data elements come (e.g., Vital Signs or Mental Health Assessment).6
2.1 Types of information in Fee Basis data
Below we describe the general types of information in both the SAS and SQL data. All SAS variables are denoted in capital letters, while SQL fields are denoted without spaces, in accordance with how these fields are labeled in the SQL tables.
2.1.1 Geographic variables
There are 3 categories of geographic data: veteran-related information, vendor-related information and VA-station related information. VA-station related information includes STA3N, STA6A and STANUM in SAS and Sta3n and PrimaryServiceInstitution in SQL. These variables relate to the VA station at which the Fee Basis care requests and claims are input. These geographic variables indicate the VA station paying for the service.
In SAS data, there is also a primary service area variable (HOMEPSA) that indicates the station to which the Veteran’s residence is assigned based on geography. It is not necessarily the station at which the Veteran receives most VA care or the station which will pay for a particular Non-VA Medical Care service. To locate the facility at which the Veteran usually receives VA care, the VA Information Resource Center (VIReC) recommends consulting the preferred facility indicator in the VHA Enrollment Database.7
There are also variables pertaining to Veteran geographic information, particularly ZIP, HOMECNTY and HOMESTATE in the SAS data and County, Country, Province, and State in the SQL data. With additional permissions, researchers can also access City, Postal Code, Street Address, and Zip. Researchers will need to link to the Patient and SPatient domains to access this geographic information in the SQL data.
SAS and SQL also have several geographic fields related to the vendor providing the non-VA care, such as the vendor’s city, county, state and zip code. In SAS, these data can be found in the Vendor file. In SQL, these variables can be found in the [Dim].[FeeVendor] table. Users of the data should keep in mind that these data represent the physical location of the entity billing for care, which may or may not be the same as the provider’s location.
2.1.2 Financial variables
The Fee Basis files’ primary purpose is to record VA payments to non-VA providers. Non-VA providers submit claims for reimbursement to VA. These clams contain charges and are known as claimed amounts (PAMTCL in SAS, ClaimedAmount in SQL). VA evaluates these claims and decides how much to reimburse these providers for care. Details about the VA rules governing reimbursement can be found in Chapter 7 of this guidebook.
There are two important variables to consider if evaluating the cost (VA reimbursement) of Fee Basis Care: the payment amount (AMOUNT in SAS, PaidAmount in SQL) or the Financial Management System (FMS) disbursed amount (DISAMT in SAS, DisbursedAmount in SQL). The FMS disbursed amount is the payment amount plus any interest payment. Care provided under contract is eligible for interest payments. Thus the variable INTIND (interest indicator) equals ‘1’ if the claim is eligible for interest and ‘0’ otherwise. The amount of interest paid on the claim, if any, appears as the variable INTAMT. INTIND and INTAMT are not always concordant. For example, there are observations in which INTIND = 1 and INTAMT = $0. Prior to FY 2007, INTAMT has two implied decimal places. For example, an interest payment of $14.21 would appear as ‘1421.’ INTAMT is part of DISAMT; it should not be added to them.
In general, we recommend using the disbursed amount to capture the cost of care for two reasons. First, it includes both the payment amount and any interest that may apply. Second, there are some cases where the disbursed amount is $0, while the payment amount is greater than $0; these are cases in which the payment was cancelled and the true cost of care is thus $0. If using payment amount, one would overestimate the cost of care. However, there is one situation in which the payment amount will be more accurate than the disbursed amount: when the disbursed amount is missing, and the payment was not cancelled, one should use the payment amount to capture the cost of care. Thus, our recommendation is as follows:
Use disbursed amount to calculate the cost of care, except in the case where disbursed amount is missing and the payment was not cancelled. In that case, use payment amount instead.
In the SAS data prior to FY 2007, the disbursed amount (DISAMT) had an implied decimal point whereas the payment amount (AMOUNT) did not. For example, DISAMT=1000 in FY06 really indicates DISAMT=10.00.
The amount claimed (PAMTCL) appears in the inpatient (INPT) file alone; there is no claimed amount on the outpatient side.
The specific locations of the SAS payment variables and the SQL payment variables can be found in Chapters 4 and 5, respectively.
2.1.3 Time to process claims
There are delays in the processing of Fee Basis claims. Thus, researchers using later years of data should be aware that files are not static and will continue to be updated. For example, accessing FY2014 data on Dec 1, 2014 will likely result in fewer observations than when accessing FY 2014 data on Dec 1, 2015.
To evaluate the time it takes VA to process Fee Basis claims, we evaluated SAS data for FY2014. We compared the service date (TREATDTO in inpatient and ancillary, TREATDT in outpatient, and FILLDTE in pharmacy files) to the FMS processing date (PROCDTE) (See Table 1). More than 99% of claims for inpatient, ancillary and outpatient care are processed within 2 years. Given these delays in processing claims, we recommend that analyses use Fee Basis data from 2 years prior to the current date to ensure almost complete capture of inpatient, ancillary and outpatient data.
2.1.4 Inpatient data
Inpatient stays in both SAS and SQL Fee Basis data can denote hospital stays, nursing home stays, or hospice stays. VA contracts out its hospice; therefore, the Fee Basis files contain a great deal of data related to hospice care.
As noted earlier, there are often multiple records that indicate a single inpatient stay – each record pertains to a unique invoice number. Fee Basis providers vary in how frequently they submit an invoice for Fee Basis care. In FY 2014, the longest length of stay associated with a single nursing home invoice was 31 days. Most nursing home care is billed monthly, so there is one claim for each month of nursing home stay. Hospice also appears to be billed monthly, with longest length of stay for a single hospice invoice of 31 days. The length of stay for a single hospital invoice varied greatly, with a maximum length of stay of 980 days. However, 99% of inpatient hospital invoices were associated with a length of stay of 33 days or less.
In order to evaluate the care received, length of stay and/or costs associated with a single inpatient stay, the user will often have to roll up multiple claims. This can become complicated by the fact that not all encounters relating to the same inpatient stay will have the same admission and discharge dates. For example, a hospital stay may last from Jan 1, 2010 to Jan 10, 2010, and have another claim for treatment provided on Jan 5, 2010. In this case the first record would have an admission date of Jan 1, 2010 and a discharge date of Jan 10, 2010. The second record would have an admission date of Jan 5, 2010 and a discharge date of Jan 5, 2010. Thus, one could not simply use the patient identifier and the admission and discharge dates to collapse these observations into one inpatient stay. (In SAS the admission date is denoted by the TREATDTF variable and the discharge date by the TREATDTO variable, in SQL the admission date is denoted by the AdmissionDate field and the discharge date is denoted by the DischargeDate field).
We present here one way to collapse records into a single inpatient stay, but users may wish to develop their own method specific to the research question at hand. We assume here that new inpatient stays are defined by a change in vendor or a gap in treatment day more than 1 day.
Steps to collapse records into a single inpatient stay:
1. Sort data by the patient ID, STA3N, VEN13N, and the admission dates.
a. In SAS, the Patient ID will be the SCRSSN and the admit date is the “treatment from” date.
b. In SQL, the patient ID will be the PatientICN or PatientSID, and the admit date is the “admission date.”
2. Compare the discharge date of the first observation to the admission date of the next (second) observation. If the gap is 0 or 1, evaluate the discharge date of the first and second observation. The “temporary end date” is the maximum of these two values.
3. Compare the admission date of the third observation to the “temporary end date” from above. If the gap is 0 or 1, it is part of the same hospital stay and we then want to assess its discharge date. The new “temporary end date” is the maximum of the discharge date of the third observation and temporary end date from Step 2.
4. We continue on this process until we find a gap greater than 1 day or we have evaluated all observations with that patient ID, STA3N and VEN13N.
5. Once the process is exhausted for a particular patient, STA3N and VEN13N combination, we calculate length of stay as the difference between the admission date of the first record and the “temporary end date.”
6. All observations for this particular patient ID, STA3N and VEN13N where the admission date comes on or after the admission date of the first record AND the discharge date comes on or before the temporary end date are considered to be part of the same inpatient stay.
7. Move on to the next patient ID, STA3N, VEN13N combination and repeat the entire process above.
A single inpatient encounter may generate zero, one, or multiple ancillary records, depending on the number of ancillary procedures and physician services received.
Previous work conducted for the HERC 2008 Fee Basis guidebook found that the cost of inpatient pharmacy was included in the inpatient records of the SAS INPT file.
2.1.5 Outpatient data
In both SAS and SQL data, outpatient data are organized in long format, with one record per CPT code. Unlike the inpatient data, there can be multiple records with the same invoice number. For example, if a physician billed for a complete blood count and a venipuncture in the same day, there would be two records with the same invoice number, but different CPT codes and different claimed amounts. Some encounters have multiple procedures that are paid as a single encounter; other encounters have multiple procedures and there are separate payments for each procedure.
As a single encounter may have more than one CPT code, users may have to aggregate multiple observations in order to evaluate the care received on a particular day. One way to do this is to concatenate the vendor identifier, the patient identifier, and the visit date. Please note that this method providers an indication of the care provided to a Veteran on a single day, rather than in a single encounter, because multiple providers may use the same billing vendor. If a patient saw two different providers on the same date who use the same vendor for billing, it will not be possible to distinguish the two encounters.
2.1.6 Pharmacy data
There is very limited outpatient pharmacy data in the Fee files. VA patients who receive prescriptions from non-VA providers fill them from a VA pharmacy, often the VA Certified Mail Order Pharmacy (CMOP). The prescriptions filled by fee-basis pharmacies are often small quantities of medication to meet the patient’s emergency or short-term needs while a CMOP prescription is being filled. Each prescription record has a fill date and a patient identifier (either PatientICN or scrambled social security number). The outpatient pharmacy data includes medications dispensed in a pharmacy. Medications dispensed in a health care facility such as a doctor's office, dialysis clinic, or hospital outpatient clinic, such as injectable medications or infusions, will be found in the outpatient data, where they will be identified by CPT code.
2.1.7 Type of care variables
There are a number of different variables that denote the category of care a Veteran received through Fee Basis (see Table 2) Appendices B and H present more details about the values these variables can take. The Fee Purpose of Visit Code (FPOV) has strong guidance from VA Fee Basis Office and thus may be a more accurate way of categorizing care.
One exception to this is when identifying emergency department (ED) visits. If researchers wish to identify ED visits, they may want to use CPT codes or Place of Service codes, rather than FPOV. This is in line with the way VHA Office of Productivity, Efficiency & Staffing (OPES) ascertains ED visit. More information can be found at the OPES website: http://opes.vssc.med.va.gov (VA intranet only). If a researcher decides to use FPOV, please note that an FPOV value of 52 indicates ED visit for persons whose care is covered under the Millennium Bill and should thus be included in evaluating ED care. FPOV values of 32 and 33 also indicate ED visits, but are only observed in the Ancillary file. Most ED visits will be identified through FPOV values of 32 or 33.
2.1.8 Vendor and provider variables
Each observation in the SAS and SQL data has an accompanying vendor ID. The vendor represents the entity billing for the non-VA care, while the provider represents the person who was involved in care provision. The vendor and the provider may or may not be the same entities. There may be many providers that use the same vendor for billing. If there are multiple providers using the same entity to bill their claims, it will not be possible to disaggregate what type of provider the patient saw (e.g., an internal medicine physician or an infectious disease specialist). SAS and SQL contain different variables to identify the provider and/or vendor associated with the care.
In both SAS and SQL, it can be difficult to determine the provider the Veteran saw for Fee Basis care. There are very limited data in both the SAS and the SQL Fee Basis data regarding the provider associated with care; the closest one can get to this information is to denote the vendor associated with the encounter (detailed more in sections 4.11 and 5.10). This is true for both the inpatient and outpatient data.
In both SQL and SAS data, there is also a variable regarding the fee specialty code. These data indicate the specialty code associated with the vendor, such as orthopedic surgery, cardiology, family practice, etc. However, in all data files, the vast majority of observations are missing values for this variable.
It can be difficult to identify the specific type of provider associated with Fee Basis care in the currently available national extracts of Fee Basis data.
2.1.9 Travel data
Veterans who meet certain criteria may be eligible for mileage reimbursement for travel to and from VA or Non-VA care. As of July 2015, the current mileage reimbursement rate is 41.5 cents per mile. In order to qualify for round trip mileage, an appointment must be scheduled. Unscheduled trips may be reimbursed for the return mileage only. The mileage is calculated using the fastest route. For more information, including information on deductibles and special transports, visit: https://www.va.gov/health-care/get-reimbursed-for-travel-pay/.
2.2 Apparent data anomalies
HERC investigation of Fee Files reveals certain data anomalies of which researchers should be aware.
There may be multiple vendor IDs (VENDIDs) for a single inpatient stay. This could indicate a transfer between facilities or a physician bill for an inpatient stay. Note that some physicians use the same ID number as the hospital.
There may be multiple STA3Ns for a single inpatient stay. This rare event most likely indicates a transfer.
In some cases it may appear that single encounters have duplicate payments. However, investigation has confirmed these are partial payments made for a single encounter or procedure.
Facility charges vs. ancillary charges: There are instances when there may be claims for facility charges with no corresponding ancillary provider charge. For example: services provided at a hospital anticoagulation clinic are billable for facility charges only if the anticoagulation is considered ‘incident to’ physician services and certain other conditions are met.8
In some cases it may appear that single encounters have duplicate payments. However, previous HERC investigation confirmed these are partial payments made for a single encounter or procedure.
Pre-2007, DISAMT and INTAMT each have two implied decimal places – a value of 1000 would indicate $10.00.
_____________________________________________________________________________
Notes and Recommendations
- Each year represents the year in which the claim was processed, not the year in which the service was rendered.
- When evaluating the cost of care, use the disbursed amount. If disbursed amount is missing (but not $0), use payment amount instead.
- There are often multiple observations per inpatient stay and multiple observations per outpatient encounter. Researchers and analysts will have to take care to collapse observations properly if warranted, for example to determine the costs, procedures or diagnosis associated with a single stay or visit.
- There are limited data available regarding the specific non-VA provider associated with a visit; much information available pertains to the vendor who is billing for the care provided.
- However, there are data available regarding the category of visit. Fee Purpose of Visit is the recommended way to evaluate the category of the visit.
_____________________________________________________________________________
3. How SQL versus SAS data differ
SAS versus SQL data differ in three main ways:
1. how they are organized
2. how they are accessed
3. the variables they contain
Appendix A lists all variables in the SAS files. Those with access to the VA intranet can find a list of SQL fields on the CDW MetaData site. Go to CDW Home, click on CDW MetaData, then click on the link for Purchased Care.
3.1 How data are organized
The SAS Fee Basis data are organized by fiscal year. Each year represents the year in which the claim was processed, not the year in which the service was rendered. SAS data are housed in 8 ready-to-use datasets per fiscal year. Table 3 lists their file names and gives a general description of their contents.10
SQL Fee Basis data are stored in the form of multiple relational tables that must be linked, or in SQL parlance, joined, in order to create an analysis dataset. For example, if one wishes to evaluate the cost of certain diagnoses in inpatient care through SQL data, this would require the linking of multiple tables before being able to conduct any analyses such as [Fee].[FeeInpatInvoice], [Fee].[FeeServiceProvided], [Fee].[FeeInitialTreatment], [Fee].[FeeInpatInvoiceICDDiagnosis], [Dim].[ICD9] tables. Appendix D contains information on the primary and foreign keys needed to link the various SQL tables.
3.2 Variables in the data
There are also differences in the variables contained in the SAS versus SQL data. SAS has more data on inpatient diagnosis and procedure variables than do SQL data.
Using SQL data will allow the researcher to link to other rich data found in CDW, such as the Health Factors data.
While a researcher could theoretically conduct a Fee Basis analysis using SAS data and then upload these SAS data to CDW and pull in the relevant variables from the SQL Patient domain, this poses some logistical challenges. In the SAS data, the patient identifier is the scrambled social security number (SCRSSN). SQL data contain both SCRSSN and SSN, but these data reside in the SPatient table at CDW, and cannot be accessed by researchers without the CDW data manager and IRB approval. The unique patient identifier by which to conduct SQL-based Fee Basis analyses is PatientICN. Researchers will thus need permissions to allow the CDW data manager to obtain SCRSSN or SSN to PatientICN crosswalk to allow for the necessary data linkages. Researchers using this tactic also run the risk of not being able to properly link their cohort, as other HERC investigations have revealed an imperfect relationship between SCRSSN and ICN; some SCRSSNs do not have an accompanying PatientICN; some SCRSSNs have multiple PatientICNs.
Patient identifiers are also different across SAS and SQL data. As noted above, in SAS, the patient identifier is the SCRSSN; this is unique to each patient across the entire VA. In SQL, there are multiple patient identifiers, with the most useful being the PatientICN. Unlike the other patient identifiers in SQL such as PatientIEN or PatientSID, PatientICN is supposed to be unique to each patient across VA. Given these different patient identifiers, it is difficult to conduct exact comparisons between SAS and SQL data. However, in Table 4, we present some comparisons to demonstrate the different between SAS and SQL data.
3.3 Observations contained in the data
It is also possible that researchers will find a slight difference in the observations that the SAS versus SQL data contain. As noted above, there are differences in the patient identifier and the date variables in the SAS versus SQL data; both data sources do not contain the same variables regarding patient identifier or date the claim was paid. Therefore, it is not possible to do an exact comparison across the datasets. However, we conducted some comparisons for inpatient data. For the inpatient data, we compared observations with the same patient identifier, based on PaidDate in SQL and TRANSDAT in SAS. We crosswalked the ScrSSN to allow for comparison with SAS data. Data are presented in Table 4.
Researchers will notice a high degree of concordance between SAS and SQL data in most years of analysis. Data from FY1998 and FY1999 have a greater degree of discordance.
3.4 Inpatient data in SAS versus SQL
There are substantial differences in quantity of inpatient diagnosis and procedure data available in SAS versus SQL. SQL inpatient data contain up to 5 diagnoses and 5 procedure codes, while SAS inpatient data contain up to 25 diagnosis codes and up to 25 procedure codes. SAS data also contain an additional diagnosis variable that is not present in the SQL data -- DXLSF. The definition of the DXLSF variable changes depending on the year of analysis. Up to FY2008 data, DXLSF is labeled as “1st Diagnosis Code.” In FY2009 and on, DXLSF is labeled as the “Admitting or Primary Diagnosis Code.” In FY 2009 and later SAS data, there is also another variable, DX1, which is not present in SAS data prior to FY2009. This variable is defined as ‘1st Diagnosis Code.” A comparison from FY 2009 to 2014 data reveals that DX1 in SAS corresponds to DX1 in SQL data, and up to 2008, DXLSF in SAS corresponds to DX1 in SQL (see Table 5). Other work by HERC researchers indicates that in the FY 2014 data, DXLSF and DX1 were identical 47% of the time.
Given the variable definitions, it is not clear whether DX1 or DXLSF is the better choice to determine primary reason for inpatient stay. Researchers evaluating care over time may want to use the DRG variable. However, one also needs to exercise caution with DRG; there are 2 different sets of DRGs used over time. PMS-DRG was effective in FY 2008; prior to this time CMS-DRGs were used. The 2 sets of DRGs are not interchangeable. For example, the meaning of DRG001 is not the same in FY05 vs FY15. In FY05, DRG001 means “CRANIOTOMY- >17 W CC”, compared to “HEART TRANSPLANT OR IMPLANT OF HEART ASSIST SYSTEM W MCC” for DRG001 in FY15 DRG001.
There are different ways of costing out an inpatient stay in SAS and SQL data. In SAS, the cost of an inpatient stay can be determined by summing the cost from DISAMT in the inpatient files with the DISAMT from the ancillary observations that correspond to the inpatient stay; however, the inpatient and ancillary files alone may not be sufficient to account for the entire cost of care. HERC researchers found that claims for the professional component of hospital stays also appeared in the file of claims for outpatient services. Therefore, to make a complete assessment of the payments for inpatient cases, researchers should evaluate the outpatient files along with the inpatient and ancillary files. In the SQL files, there is no separate ancillary file; rather, data regarding the physician cost of the inpatient stay is denoted in the [Fee].[FeeServiceProvided] table. Thus, in SQL the total cost of an inpatient stay would be determined by evaluating the DisbursedAmount in the [Fee].[FeeInpatInvoice] and [Fee].[FeeServiceProvided] tables.
3.5 Outpatient data in SAS versus SQL
In SAS, the outpatient data are housed in the MED files. In SQL, the outpatient data are housed in the FeeServiceProvided table. However, not all data in the FeeServiceProvided table are outpatient data; some may pertain to inpatient stays. Researchers will have to select observations from the SQL FeeServiceProvided table in order to ensure they are only evaluating outpatient data. Researchers can do this using the FeePurposeOfVisit (FPOV) code.11 We recommend this approach over using another variable, such as the Fee Program. In this table, some ancillary data are associated with an inpatient FPOV code but have an outpatient FeeProgramProvided field. Given the stronger guidance from the Fee Office regarding use of the FPOV code, we recommend using the FPOV code to discern which observations are ancillary care, as the FeeProgram may not be as reliable. Appendix G lists all available FPOV codes and classifies them as inpatient or outpatient.
_____________________________________________________________________________
Notes and Recommendations
- Fee Basis data are housed in both SAS and SQL format. Researchers will need to decide whether they will use the SAS or the SQL data and apply for appropriate IRB approval for use.
- SAS and SQL data are organized differently and contain different variables. There is a strong, but imperfect, concordance, between the observations housed in the SAS and SQL data.
______________________________________________________________________________
4. SAS Data
4.1 Overview
The data files in each fiscal year represent all claims processed in the FMS during the year. They do not represent all claims received during the year. Most importantly, they do not represent all care provided during the fiscal year. This is a critical difference from VA utilization files, which are organized by date of service. To find all care provided in a particular fiscal year requires searching by treatment date over several years of Non-VA Medical Care claims.
There is no official data dictionary for the SAS Fee Basis data. We therefore use the PROC CONTENTS to describe SAS variables, found in Appendix A.
4.2 Patient identifiers in SAS
SAS data use patient scrambled social security number (SCRSSN) as the patient identifier.
4.3 Inpatient data in SAS
In SAS, the cost of an inpatient stay can be determined by summing the cost from DISAMT in the inpatient files with the DISAMT from the ancillary observations that correspond to the inpatient stay; however, the inpatient and ancillary files alone may not be sufficient to account for the entire cost of care. HERC researchers found that claims for the professional component of hospital stays also appeared in the file of claims for outpatient services. Therefore, to make a complete assessment of the payments for inpatient cases, researchers should evaluate the outpatient files along with the inpatient and ancillary files.
4.4 Demographic data in SAS
SAS data have limited patient demographic data. The Veteran files contain the richest patient demographic information in the SAS data; these include the Veteran’s date of birth, sex, prisoner of war status and war code. The SAS files also include a patient type variable (PATTYPE). Patient type can take one of seven values: surgical; medical; home nursing; psych contract; psychiatric, neuro contract; or neurological. SAS Fee Basis data can be linked to other SAS files with additional demographic data (e.g., Vital Status files, enrollment files).
4.5 Clinical data in SAS
Clinical variables in SAS format include ICD-9 diagnosis codes, ICD-9 surgical codes, CPT codes and CPT modifier codes, DRG codes and Present on Admission codes.
Inpatient procedures are captured by ICD-9 procedure codes (SURG9CD1-SURG9CD25) in the hospital claims file. There is a CPT field in the inpatient files, but this is always missing; hospitals do not use CPT codes to bill.
Procedures are identified by CPT code (CPT1) in the non-hospital inpatient services (the ancillary file) and in the outpatient procedures file. Both ancillary and outpatient files have one record per CPT code.
In SAS, ICD-9 diagnosis codes are in the Inpatient, Outpatient and Ancillary files. For some years, there may be high rates of missingness of ICD-9 data in the Ancillary files. There are up to 25 ICD-9 diagnosis codes and 25 ICD-9 surgical procedure codes in the inpatient data. Starting in 2009, there are also a number of DXPOA variables in the SAS data, which indicate diagnoses that are present on admission.
In the SAS data, the provider component of the inpatient stay is captured in the ancillary file.
Six additional variables indicate the setting of care and vendor or care type. They appear in Table 6, where an ‘X’ indicates that the variable appears in the file.10 Vendor type (TYPE), payment category (PAYCAT), treatment code (TRETYPE), and place of service (PLSER) all provide information on the type or setting of care. They could form part of an overall strategy to locate care provided in specialized settings, such as state homes, or of specialized services like kidney dialysis. PLSER values overlap considerably with those of the Medicare Carrier Line Place of Service codes. The Fee Purpose of Visit (FPOV) and Health Care Financing Agency Payment Type (HCFATYPE) variables feature values pertaining to setting (inpatient, outpatient, home-based), specific items (e.g., supplies and diagnostics), and miscellaneous purposes.[1]
Values for Fee Purpose of Visit (FPOV), HCFA Payment Type (HCFATYPE), Treatment Code (TRETYPE), Place of Service (PLSER), and Vendor Type (TYPE) appear in Appendix B. New values may be added over time. Appendices G and H, copied from the Non-VA Medical Care program website, describes in detail the types of records for which each Fee Purpose of Visit (FPOV) codes are assigned.
Researchers must consider whether a missing value means “not applicable.” For example, many inpatient (INPT) records lack a value for any of the surgery codes (SURG9CD1-SURG9CD5). This most likely reflects a low frequency of surgery rather than missing data. Conversely, all stays should have at least one discharge diagnosis. A missing value of the primary diagnosis code should therefore be treated as truly missing. The same cannot be said for DX2-DX25, however, as additional diagnosis codes are optional.
4.6 Prescription data in SAS
All SAS prescription-related data is found in two files: the PHR file and the PHARMVEN file. The PHR file contains information on the cost-related data associated with the prescription, while the PHARMVEN file contains information on the vendor associated with the prescription. Prescription-related data in the PHARVEN file contain only summary payments by month. These data records cannot be linked to particular patient identifiers or encounters. Each record in the pharmacy services (PHR) file represents a single prescription, whether for a medication or a pharmacy supply (e.g., skin cleanser, bathing cloths). There is no information available in the SAS data that identifies the actual medication dispensed.
4.7 Provider data in SAS
The Medicare hospital provider ID (MDCAREID) is entered by fee basis staff in order to calculate hospital reimbursement using the Medicare Pricer software. The Medicare ID is missing if the payment is determined via a different mechanism (e.g., a contract). If a researcher wishes to find the Medicare hospital provider ID, one approach is to use the vendor identification variables (VEN13N, VENDID) to locate the vendor’s name and location in the VEN file, and then to use this information to find the Medicare provider ID using publicly available files from CMS, the agency that oversees the Medicare program. Another approach is to search other fee claims submitted by the same vendor to see if a Medicare hospital ID was assigned to those claims. For some vendors, there may be more than on possible hospital, for example, if the vendor is a hospital chain or an organization with a VA contract.
The payment category (PAYCAT) is missing for all records in the inpatient services (ANCIL) file. Missing values of PAYCAT could be imputed by finding the corresponding inpatient stay in the INPT file.
4.8 Financial data in SAS
As noted in Chapter 2, the important variables capturing cost of care are AMOUNT and DISAMT. Persons working with the SAS data should keep in mind that prior to FY 2007, the disbursed amount (DISAMT) had an implied decimal point whereas the payment amount (AMOUNT) did not. For example, DISAMT=1000 in FY06 really indicates DISAMT=10.00.
There are also a number of other financial variables denoted in SAS (see Table 7). In SAS, the inpatient (INPT) file includes PAMT, the Medicare prospective payment that would apply to the stay. VA calculates PAMT from CMS pricer software on the basis of DRG and length of stay. There are additional payments for direct medical education, capital-related costs, and other factors as appropriate. The VA payment (DISAMT) is typically less than or equal to the PAMT value, although in some cases VA will pay more than Medicare would pay. For more details, including rules for handling patients transferred during a stay, see federal regulation 38 CFR 17.55.
The payment amount variables (AMOUNT and DISAMT) are missing (blank) in a small number of cases. These represent cases in which payment is disallowed. The values of Adjustment Codes 1 and 2 (ADJCD1 and ADJCD2) explain the reason for non-payment. Appendix H lists their current values.
The Fee Card (VET) file contains only summary payment figures by month, although researchers can match the records to other data by SCRSSN and other identifiers.
The travel payments data contains reimbursements for particular travel events (TVLAMT). Through patient ID (SCRSSN) and travel date (TVLDTE) one can link these payments to inpatient and outpatient encounters.
4.9 Financial processing data in SAS
Many variables in the Fee Basis files record details of invoice and check processing. Most files contain the invoice date, obligation number; check number and date, several variables pertaining to check cancellation and denials of payment, and the DHCP internal control number. Five additional variables – Financial Management System (FMS) transaction number, line number, date, batch number, and release date – reflect processing of payments through the FMS. With few exceptions these variables will be of little interest to researchers.
4.10 Care location in SAS
Care provided to persons associated with a particular VA station can be found by selecting records by STA3N. It would seem logical to use the vendor’s location, found in the vendor files PHARVEN and VEN, to associate care with a particular station, but this should be approached with caution. Some vendors use centralized billing services located in other cities, in a few cases in other states. Thus, the mailing address of the vendor is not always the vendor’s actual location.
Several variables are available for locating care in particular settings. These include Fee purpose of visit (FPOV), place of service (PLSER), type of treatment (TRETYPE), HCFA payment type (HCFATYPE), and record type (TYPE). Not all of these variables appear in every utilization file. Because coding varies by station, users are encouraged to employ multiple variables in an effort to find all care associated with a particular setting or service type.
If the patient was transported to a VA hospital after stabilization (as indicated by the DISTYP, or disposition type, variable), the record of the VA stay should appear in VA utilization databases. If it cannot be located in the PTF Main file or DSS NDE for inpatient care, search other inpatient files. If it still cannot be found, then the stay may have ended on the day the person stabilized.
4.11 Provider/vendor data in SAS
There are multiple potential identifiers for provider/vendor in the SAS data: the VENDID, VEN13N, MDCAREID, SPECCODE and NPI.
The vendor identity can be found through the VENDID or VEN13N variables in SAS. VENDID is the vendor ID. The VEN13N is the vendor ID with a suffix; VEN13N is more detailed than VENDID and is thus recommended for use. Multiple SAS datasets have VENID and VEN13N. While there is limited information about the vendor available in the SAS datasets; the most comprehensive information about the vendor can be found in the SAS VEN and SAS PHARVEN datasets. The SAS PHARVEN dataset contains information only about pharmacy vendors. Note that the vendor may represent the hospital, a hospital chain or the entity billing on behalf of the provider.
MDCAREID is the Medicare OSCAR number, which is a hospital identifier. In some cases, there is a one-to-one relationship between VEN13N and MDCAREID. If this is the case, then it can be assumed that any care provided by the vendor with that VEN13N is actually a hospital with that MDCAREID. For some VEN13N, however, there is more than one MDCAREID. These vendors are presumably hospital chains. Some VA medical centers purchase care from only one of the hospitals in the chain. If that analyst examines VEN13N and STA6A (in inpatient Fee Basis data, this field represents the VA hospital arranging care), there is often only one MDCAREID. In this situation, a given VA medical center has a preferred hospital from which it purchases care. To determine the location of care, MDCAREID will be more useful than VEN13N. The zip code accompanying the VEN13 variable denotes the zip code to which VA sent reimbursement, not the zip code where the service was rendered. In VA datasets, the MDCAREID does not have an accompanying address, but one can use other non-VA datasets (e.g., Hospital Compare) and determine the address of the hospital’s physical location through the common MDCAREID variable.
MDCAREID is available in most inpatient SAS Fee Basis records. There are exceptions. It is not available for claims in which payment was based on a contract amount. MDCAREID is not available in the outpatient SAS Fee Basis data, even though some outpatient services are provided in a hospital. When MDCAREID is not available, it is possible to assign MCCAREID based on the relationship between VEN13N and STA6A. In this way, records that are missing MDCAREID can be given a MDCAREID based on the value of VEN13N and STA6A in the record. This is helpful in determining the location of care in inpatient claims in which MDCAREID is missing, and in outpatient claims for hospital-provided services.
The NPI is the national provider identifier, which is provider-specific but often missing in the Fee Basis data. Analyses of FY 2014 data indicate approximately 50% of inpatient observations and 43% of outpatient observations are missing NPI. Among non-missing observations, HERC analyses found a many-to-many relationship among NPI and VEN13N. For example, there could be many NPIs associated with a VEN13N (e.g., a hospital employing multiple providers), or many VEN13Ns for a single provider (e.g., a surgeon with privileges at multiple hospitals).
Medical specialty type (SPECCODE) is a provider-specific variable and indicates the specialty type of the provider rendering the service. It is available in the PHARVEN and VEN files, albeit with a high degree of missingness.
____________________________________________________________________________
Notes and Recommendations
- The same concept (such as fiscal year, state, or county) may be represented by several variables, sometimes in differing formats.
- Missingness can vary substantially by year and by file. Some missingness may indicate “not applicable.”
- It can be difficult to determine the provider and the location of the Non-VA care provider.
______________________________________________________________________________
5. SQL Data
5.1 Access
SQL data are housed at CDW, which is a collection of many servers. Table 8 denotes on which CDW servers Fee Basis data are housed. Researchers can read more information about accessing CDW on the VHA Data Portal (http://vaww.vhadataportal.med.va.gov/DataSources/CDW.aspx; VA intranet only).
5.2 Overview
SQL data must be linked from multiple tables in order to create an analysis dataset. SQL tables can be joined through linking keys. There are two types of keys: primary keys and foreign keys. A primary key is a key that is unique for each record. Each table has only one primary key field. A foreign key is a key that uniquely identifies a record of another table.
We give an example here that relates to FeeInpatInvoice table. This table contains information on inpatient care. The codes for the procedures provided for a given hospital stay are kept in a separate table, a table of procedures.
To understand what procedures were performed during an inpatient stay in the [Fee].[FeeInpatInvoice] table, one must first link that table to the [Fee].[FeeInpatInvoiceICDProcedure] table. The key that allows for this linkage is the “FeeInpatInvoiceSID” which is a primary key in the [Fee].[FeeInpatInvoice], and a foreign key in the [Fee].[FeeInpatInvoiceICDProcedure]. Then, to see which ICD procedure codes were coded for this inpatient stay, one must link to the [Dim].[ICDProcedure] table through the ICDProcedureSID. Here, ICDProcedureSID is a primary key in the [Dim].[ICDProcedure] table and a foreign key in the [Fee].[FeeInpatInvoiceICDProcedure] table.
This seeming complicated arrangement is an efficient way to store data. The procedure code table has just as many records as there were procedures on the invoice. The key field indicates which invoice they appeared on. The alternative, putting the procedure code fields in the invoice table, would not be as efficient. The invoice table would have to have a sufficient number of fields to accommodate the maximum number of procedures report on any invoice. Most of these fields would be empty. By store procedure codes as records in another table, the SQL relational database uses the minimum amount of storable space. A record is created only if there is a code on the invoice to be recorded. Before working with any SQL tables in CDW, we recommended familiarizing yourself with the schema diagram in order to understand how to link tables to one another. The Fee Basis schema data can be found at the CDW SharePoint portal at the links below (VA intranet only). Primary keys are denoted by (PK) and foreign keys are denoted by (FK).
URLs are not live because they are VA intranet only. Researchers with VA intranet access can access these images by copying and pasting the URLs into their browser.
Authorized:
https://vaww.cdw.va.gov/metadata/Reports/ERDiagramsOfViews/Purchased%20Care%20Authorized_5638.jpg
Unauthorized:
https://vaww.cdw.va.gov/metadata/Reports/ERDiagramsOfViews/Purchased%20Care%20Unauthorized_242.jpg
Service:
https://vaww.cdw.va.gov/metadata/Reports/ERDiagramsOfViews/Purchased%20Care%20Service_5480.jpg
While Unauthorized care is considered a separate domain, the data pertaining to Unauthorized care are stored alongside the Authorized care data in the FeeInpatInvoice table and the FeeServiceProvided table. One can evaluate which encounters were unauthorized by joining the FeeUnauthorizedClaim table through the FeeUnauthorizedClaimSID key.
Of note, the relevant SQL tables for Fee Basis data are not only the [Fee].[XXX] tables, but also the [DIM].[XXX] tables.9,12 Tables under the DIM schema contain attributes that describe the records in the Fee tables. A Fee table will contain a record for an ICD-9 code, whereas a DIM table will contain the possible values of that ICD-9 code. For example, to understand the ICD-9 codes associated with a particular inpatient encounter, one would have to link the [Fee].[FeeInpatInvoiceICDDiagnosis] with the [Dim].[ICD] table, the latter of which contains a list of all possible ICD-9 codes. Some important DIM tables that will be useful in analyzing Fee Basis data are FeePurposeOfVisit, FeeSpecialtyCode, FeeVendor, ICD, ICDProcedure Code, DRG, CPT, and CPT Category.
The CDW SharePoint site has a document that lists the purchased care SQL tables, the fields of that they contain, and some sample SQL queries (VA intranet only: https://vaww.cdw.va.gov/metadata/Metadata%20Documents/Forms/AllItems.aspx). Documentation, including data contents, field frequencies, and record counts, is also available on VIReC’s CDW Data Documentation page (VA intranet only: http://vaww.virec.research.va.gov/CDW/Documentation.htm).
5.3 Working with patient identifiers in SQL
There are five forms of patient identifiers in SQL files at CDW (including but not limited to the Fee Basis files): PatientICN, PatientSID, PatientSSN, ScrSSN, and PatientIEN. Table 1 in the Data Quality Analysis team’s guide “Linking Patient Data in the CDW Update” provides a brief summary for each identifier (Available at the VHA Data Portal. VA intranet only: http://vaww.vhadataportal.med.va.gov/Resources/DataReports.aspx).
PatientIEN and PatientSID are found in the general Fee Basis tables. PatientIEN and PatientSID are unique to a patient within a facility, but not unique to a patient across VA facilities (e.g., a patient who had visited multiple VA facilities will have multiple PatientIENs and multiple PatientSIDs). The PatientSID is a CDW assigned identifier that uniquely identifies a patient within a facility. If a patient received care at another facility, that patient will be have a different PatientSID assigned for that facility. PatientIEN is assigned by the facility. It may duplicate the PatientIEN of another patient at another facility, and should not be used as an identifier.
PatientICN is assigned by CDW. It is the patient identifier that uniquely defines a patient across all facilities. Researchers should use PatientICN to link patient data within CDW. Each patient should have only one ICN in the entire VA, regardless of the number of facilities at which he is seen. Fee Basis tables, however, only list PatientSID and do not list PatientICN. Records that relate PatientSID to PatientICN are found two tables: Patient.Patient and SPatient.Spatient. VA employees working on research studies cannot create their own crosswalk file as they do not have permission to use these files. Researchers with the appropriate DART permissions can ask the study’s VINCI data manager to create a crosswalk file. VA employees working on operations studies can build their own crosswalk file as they have permission to use these file.
5.4 Defining a cohort
Defining a cohort is an activity that is different for each project and depends on the research question at hand. However, there are best practices that all SQL-based analyses should follow. Researchers who have never before used CDW are encouraged to read the VA CDW First Time Users guide, available from the VIReC website (VA intranet only: http://vaww.virec.research.va.gov/CDW/Overview.htm). CDW Data Quality Analysis Team has particular recommendations for excluding observations before beginning analyses on your cohort.13 Corporate Data Warehouse (CDW) contains dummy data as well as test patients that will need to be removed from tables before conducting analyses. In particular, CDW also recommends Patient SIDs with a value of less than 1 be deleted. When a key field is missing, SQL indicates this with a value of -1. Persons working with SPatient or Patient data are also recommended to refer to the CDW guidance about how to delete test observations. We encourage readers to seek out the latest guidance before conducting analyses, as CDW Data Quality Analysis team may have updates to this information. (Available at the VHA Data Portal. VA intranet only: http://vaww.vhadataportal.med.va.gov/Resources/DataReports.aspx).
In summary, in order to create a research cohort, one must first identify the cohort based on PatientSID, then request the CDW data manager to link the PatientSIDs in her cohort to unique PatientICNs, and finally remove test/dummy/unnecessary PatientSIDs and PatientICNs. All analyses using this cohort should use PatientICN as indicative of a unique patient.
5.5 Inpatient care in SQL
Inpatient data are housed in the FeeInpatInvoice table as well as the FeeServiceProvided table, although the latter does not contain only inpatient data. These inpatient tables have to be linked to FeeInpatInvoiceICDDiagnosis, FeeInpatInvoiceICDProcedure, FeeInitialTreatment and the appropriate DIM tables in order to understand the specific diagnoses and procedures associated with the inpatient observations in these tables. As with the SAS data, it is not straightforward to determine the cost of, length of stay or care provided during a specific inpatient stay. Multiple claims may be submitted for each inpatient stay and the various claims do not have a common identifier indicating they are all part of the same inpatient stay.
Persons looking to find the date of service should be advised that it will not be contained in the FeeServiceProvided table. One can use the FeeInitialTreatmentSID variable in the FeeServiceProvided table to link to the Fee.FeeInitialTreatment table. This latter table contains a variable called InitialTreatmentDateTime.
Please see Section 2.1.4. for HERC advice about how to collapse multiple observations to evaluate the length and cost of a single inpatient stay.
5.6 Outpatient care in SQL
Outpatient data are housed in the FeeServiceProvided table. This table also includes claims related to inpatient care and other services. We recommend researchers use the FeePurposeOfVisit codes (FPOV) codes to eliminate observations related to non-outpatient care before beginning analyses.
Again, date of service is not available in the FeeServiceProvided table. One can use the same approach as for the inpatient SQL data described above to locate the date of service.
In the outpatient data, one observation represents a single CPT code. It will often times not be possible to determine the reason for an outpatient visit, as there will be multiple observations/CPT codes that denote a single visit. As with inpatient data, researchers will need to collapse multiple observations in order to get a complete picture of the outpatient care provided on a single day.
Appendix E includes a list of SQL fields related to the type of care a patient receives.
5.7 Prescription data in SQL
The SQL prescription data are housed in the [Fee].[FeePharmacyInvoice] and the [Fee].[FeePrescription] tables. The [Fee].[FeePrescription] table contains rich information on the type of drug prescribed and dispensed, including the drug name, manufacturer, strength, quantity, date filled and charge and disbursed (payment) amount. The table can be linked to the [Dim].[LocalDrug] table through LocalDrugSID to see whether there was the generic equivalent found in the VA drug file that was dispensed to the patient. The [Fee].[FeePharmacyInvoice] table contains information on vendor, amount claimed, and amount paid. The two tables can be joined through FeePharmacyInvoiceSID.
5.8 Demographic data in SQL
SQL Fee Basis files themselves contain limited patient demographic variables, but can be linked to other SQL data.
Basic demographic variables can be found in the [Patient].[Patient], [SPatient].[SPatient] and[PatSub] tables. A description of the Patient and SPatient schema is available on the VIReC CDW Documentation webpage: http://vaww.virec.research.va.gov/CDW/Documentation.htm (intranet only). Any variable that has an “S” prefix indicates secure data and requires special permission to access; researchers should be aware of this when submitting their IRB applications and their CDW DART data access requests.
Race and ethnicity are found in the [PatientEthnicity], [PatSub].[PatientRace] tables. Persons looking to classify patients Veterans by race and ethnicity are encouraged to read VHA guidance available on the Data Reports page of the VHA Data Portal (available on the intranet at http://vaww.vhadataportal.med.va.gov/Resources/DataReports.aspx). Guidance can be found under "VHA Data Quality Program Reports."
Military service variables can be found in [PatSub],[PatientServicePeriod], [Patient].[Patient], [PatSub].[OEFOIFService]and [Dim].[POWLocation]. Persons looking to classify Veterans’ military service are encouraged to read the Data Quality Analysis Team’s guidance on Identifying Veterans in the CDW (VA intranet only: http://vaww.vhadataportal.med.va.gov/Portals/0/DataQualityProgram/Reports/Identifying_Veterans_in_CDW.pdf).14
Patient residence related geographic information is available in the [Patient].[Patient], [Spatient].[Spatient], and [Spatient].[SpatientAddress] tables.
5.9 Travel data in SQL
The travel payment data contains reimbursements for particular travel events (TravelAmount). Through patient identifier and travel date (TravelPaymentDate), one can link these payments to inpatient and outpatient encounters. The SQL tables [Dim].[ModeOfTransportation] and [Fee].[FeeTravelPayment] contain information on travel type and payment
5.10 Provider/vendor data in SQL
SQL data contain the following vendor information: NPI, FeeVendorSID, FeeVendorIEN, NPI, VendorType and FeeSpecialtyCodeName. The vendor identity can be found through the FeeVendorSID or the FeeVendorIEN variables in SQL. Multiple SQL tables contain these variables. More detailed information about the vendor can be found in the SQL [Dim].[FeeVendor] table.
The National Provider Identifier (NPI) is a unique 10 digit identifier mandated to be used in health claims under the Health Insurance Portability and Accountability Act (HIPAA). At the time of this writing, the NPI number was often missing from fee basis claims. While NPI is available in SQL data, it does require special permissions to access, as it is located in the [Sstaff].[ SFeeVendor] table. Data in any of the any “S” tables require Staff Real SSN access. This schema contains sensitive information such as SSNs, bank accounts, and the actual name of personnel. HERC did not investigate use of NPI for this guidebook.
In SQL, there are additional variables that will denote the type and location of the care provided along with the vendor. The VendorType contains information about whether the service was provided by a laboratory, radiology, physician, pharmacy, other, travel, prosthetics, federal hospital, public hospital or private hospital. The FeeSpecialtyCodeName contains information on the specialty of the provider seen, such as oncology, chiropractic, pathology, neurosurgery, etc., but is missing much data.
5.11 Financial data in SQL
As with the SAS data, the important variables in the SQL data are the AmountPaid and the DisbursedAmount. The disbursed amount should be used to calculate the cost of care, except in the case where disbursed amount is missing. If disbursed amount is missing, use payment amount instead.
Table 9 lists a number of financial variables the SQL data contain.
_____________________________________________________________________________
Notes and Recommendations
- SQL tables require linking before conducting any data analyses. The process of linking can be complex; analysts should take care to reduce errors during this process.
- Consult the latest CDW schematic diagrams to understand the tables in which your variables of interest are housed and the primary key and foreign keys needed to link each pair of tables.
- Researchers interested in linking SQL Fee Basis data to the rich patient-level or vendor and/or provider information available in the rest of the Corporate Data Warehouse should apply for permissions to access these other datasets.
_____________________________________________________________________________
6. Access
Non-VA Medical Care data are available in SAS form at the Austin Information Technology Center (AITC) and in SAS form and SQL form through the VA Corporate Data Warehouse (CDW)/VA Informatics and Computing Infrastructure (VINCI). At the time of writing (October 2015), only operations staff will have permission to access the SAS data at VINCI. Summary data are also available through the VHA Support Services Center (VSSC) website on the VA intranet. Detailed information about accessing each of these data sources is available at the VHA Data Portal (VA intranet only: http://vaww.vhadataportal.med.va.gov).See Table 10 for a summary of the data sources.
Persons who wish to access data in the secure tables on CDW (denoted by a “S” prefix) must complete a “Real SSN Access Request Form.” This form must be signed by the IRB and Associate Chief of Staff for Research and submitted with the DART data request. For more information, please visit the Data Access Request Tracker (DART) Request Process page on the VHA Data Portal (VA intranet only: http://vaww.vhadataportal.med.va.gov/DataAccess/DARTRequestProcess.aspx#resources).
6.1 Austin Information Technology Center (AITC)
Austin Information Technology Center (AITC) is one of the VA’s five national data centers. In order to gain access to the AITC mainframe, VA system users must contact their local Customer User Provisioning System (CUPS) Points of Contact (POC) and submit a VA Form 9957 to create a Time Sharing Option (TSO) account. Facility Information Security Officers (ISOs) are often the CUPS POC. Once the VA system user has a TSO account, s/he may connect to the AITC mainframe through the Attachmate Reflection File Transfer Protocol (FTP). Additional information on accessing the AITC mainframe is available on the VHA Data Portal (VA intranet only: http://vaww.vhadataportal.med.va.gov/Home.aspx).
6.2 CDW/VINCI
SQL Fee data are available through the VA Corporate Data Warehouse (CDW)/VA Informatics and Computing Infrastructure (VINCI). Research requests for data from CDW/VINCI must be submitted via the Data Access Request Tracker (DART) application. DART is a workflow application that guides users through the request by collecting the appropriate documents, distributing documentation to reviewers, and assisting in communication between requestors and reviewers. Detailed instructions and documentation required for DART data requests can be found on the VHA Data Portal intranet website at http://vaww.vhadataportal.med.va.gov/DataAccess/DARTRequestProcess.aspx.
6.3 Web-based access
Non-VA Medical Care data may be tabulated at the VHA Support Services Center (VSSC) (VA intranet only: http://vssc.med.va.gov/). VSSC provides numerous relevant web reports, data resources, and analytics support, including summary data by facility and VISN and national summary data. VSSC web reports are organized into nine domains: Business Operations, Capital & Planning, Clinical Care, Customer Service, Quality & Performance, Resource Management, Special Focus, Systems Redesign, and Workload. Two domains in which researchers can find reports on Non-VA Care are Resource Management and Workload.
Some web reports contain PHI and access to these is restricted. Visit the VHA Data Portal for further information on accessing restricted VSSC web reports.
7. Institutional Aspects of the Non-VA Medical Care System
Using the Non-VA Medical Care data for research requires a basic understanding of laws and regulations that govern it. This section describes two elements of the program: the range of services covered and the payment rules used to determine the amount that VA will pay (DISAMT). Additional information appears in a federal regulation, 38 CFR 17.52.
7.1 Coverage
The Non-VA Medical Care program covers the full range of medical and dental care, with these exceptions:
- Care for dependent children, except newborns, in situations where VA pays for the mother’s obstetric care during the same stay. The Caregivers and Veterans Omnibus Health Services Act of 2010 (Public Law 111-163) authorizes VA to provide post-delivery and routine care to a newborn child of qualifying women Veterans receiving VA maternity care for up to seven days following the birth. Prior to the passage of this law on May 1, 2010, VA did not cover the cost of health care provided to dependent children, including newborns in situations where VA pays for the mother’s obstetric care during the same stay.
- Inpatient care beyond the time when a patient is stabilized and can be transferred to a VA facility, except where a VA facility is not feasibly available.
- Care provided in foreign countries other than the Philippines.
- Inpatient care, regardless of patient’s health status, if VA was not notified within 72 hours of admission. This rule applies even when the patient is incapable of making a call. (Veterans may submit unauthorized claims, however, and VA has legal authority to pay them under certain conditions. See 38 USC 1725 and 1728.)
- A claim for which the Veteran had coverage by a “health plan” as defined in statute. Health plans include private health insurance, Medicare, Medicaid, and other forms of insurance that will pay for medical treatment arising from the patient’s injury or illness (e.g., automobile insurance following a car accident). The generosity of the coverage is immaterial; if it covers any part of the provider’s bill, then VA may not pay anything. If the Veteran has insurance, VA cannot pay even when the entire claim is less than the deductible. If a Veteran has only Medicare Part B or has both Medicare Parts A and B, no VA payment may be made. If a Veteran has only Medicare Part A then VA may consider payment for ancillary and professional services usually covered under Part B. This is specific to certain claims for Non-Service Connected emergency medical care under Title 38 USC 1725.
- Outpatient prescriptions beyond a 10-day supply. The prescription must be for a service-connected condition or must otherwise have specific approval.
- Prosthetic items. Federal law puts prosthetics into a special payment category that mandates full financial support from VA. As implemented in VA policy, it requires that VA facilities provide all necessary prosthetics, orthotics, and assistive devices (“prosthetics”) needed by patients. VA medical centers may purchase prosthetics and related items, such as clothing specialized for prosthetic limbs, and then dispense them through VA facilities. Nevertheless, the National Non-VA Medical Care Program Office (now the VHA Office of Community Care) has interpreted VHA Directive 2006-029 to preclude Non-VA Medical Care providers from receiving payment for prosthetics. The impact on inpatient and emergent care is unclear, however, as the definition of “prosthetic” in VA is so broad as to include items placed inside the body, such as internal fixation devices, coronary stents, and cardioverter defibrillators.15 Each year the Non-VA Medical Care program funds thousands of coronary angioplasties alone, many of which will include stents. This indicates that VA pays for prosthetics, broadly defined, in some circumstances.
7.2 Veteran status
Although VA utilization files contain many non-Veterans, Non-VA Medical Care files do not. There are nine situations in which Non-VA Medical Care is authorized. Seven refer explicitly to Veterans alone, while the remaining two are for diagnostic services or eligibility exams, neither of which constitutes treatment. In general, persons on active duty in the U.S. military are excluded even if they are transitioning to VA care. One may therefore assume that all patients receiving treatment through the Non-VA Medical Care program are Veterans.
7.3 Veterans Choice card eligibility
The Veterans Access, Choice, and Accountability Act (“Veterans Choice Act”), passed in 2014, expanded veterans access to non-VA care. This act expands the non-VA care veterans were able to receive before the act was passed. Under the Veterans Choice Act, eligible veterans are able to obtain outpatient care outside the VA using their Choice Card.
Eligibility criteria:
(1) A Veteran must be enrolled in VA health care16
(2) Additionally, a Veteran must also meet at least one of the following criteria.
a. The veteran must wait over 30 days past their preferred appointment date or the date deemed medically necessary by their provider
b. Driving distance between a veterans residence and their closest VA facility is over 40 miles
c. The veteran must travel by boat or plane to access the VA facility closest to their home (excluding Guam, American Samoa, or the Republic of the Philippines)
d. The veteran faces an excessive burden in traveling to a VA, including a body of water or geologic formation that cannot be crossed by road
You can find more information about eligibility on the VHA Office of Community Care website.
7.4 Payment rules
7.4.1 Elements of a claim
A Non-VA Medical Care claim is defined by four elements:
- one Veteran
- one episode of care, which can have multiple dates within the prescribed treatment
- one provider, as identified by the Tax Identification Number (TIN), and
- one setting of care (inpatient or outpatient).
The remainder of section 7.4 details payment rules as of early 2015. These rules are subject to change by statute or regulation. Users interested in learning the rules in force at a particular point in time should contact the VHA Office of Community Care.
7.4.2 Timeliness of claims submission
VA has established rules for timely filing of unauthorized and “Mill Bill” claims (i.e. Emergency claims covered under the Veterans Millennium Care and Benefits Act, Public Law 106-117); see 29 CFR 17.120 and 38 CFR 17.1004. Four FPOV (Fee Purpose of Visit) codes can be used to identify payment for unauthorized claims. Unauthorized inpatient or outpatient claims must be submitted within 90 days from the date of care.
7.4.3 Timeliness of claims payment
After a claim is submitted electronically it must be entered manually into a Non-VA Medical Care approval system. A “claims scrubber” software program is run to ensure completeness and to locate possible errors. A claim without errors or omissions is said to be “clean.” If VA has authority to pay the claim and the submitted documentation is sufficient then the claim is approved for payment. VA has set a goal of processing all clean claims within 30 days. Actual processing time has varied considerably over the years. According to the Health Administration Center Internet website, the proportion of claims processed within 30 days rose from under 40% in 2007 to over 97% by the end of 2008.
7.4.4 General payment rules
Payment guidelines for non-VA are outlined in federal regulations §17.55 and §17.56. The Non-VA Payment Methodology Matrix, prepared by the National Non-VA Medical Care Program Office (now the VHA Office of Community Care), presents guidelines for preauthorized care and emergency care for service and non-service connected conditions for both inpatient and outpatient care.17 VA will reimburse the same non-VA provider a different rate depending on whether the Veteran received: a) pre-authorized care; b) emergency care for a service-connected condition; or c) emergency care for non-service connected conditions and non-service connected Veterans.
For inpatient and outpatient care, in general, VA will pay the lesser of the Medicare rate (or MPFS rate) or the billed charges. A summary of the payment guidelines can be found in Appendix I. For more detailed information, researchers should visit the VHA Office of Community Care website.
Payment for care provided under the Veterans Choice Act may not exceed the Medicare Fee Schedule (i.e. the rates paid by the United States to Medicare providers). However, the VA may pay a rate higher than the Medicare Fee Schedule rate for care provided in highly rural areas, as long as this rate is determined to be fair and reasonable by VA. One can find more information on payment rates under the Veterans Choice Act in federal regulation §17.1500. When there is no available rate in the Medicare Fee Schedule, the VA will follow the payment guidelines for Non-VA Medical Care.
7.4.5 Travel
Many classes of Veterans are eligible for travel payments. VA will arrange for transportation for them or will reimburse expenses on the basis of vouchers submitted. Reimbursements appear in the Travel Expenses (TVL) file. There is a deductible of $3 per trip up to a limit of $18 per month. VA can waive the deductible in hardship cases. The charge for an ambulance trip to a non-VA hospital may be paid through the Non-VA Medical Care program if the medical center determines that the hospital services meet the criteria for an unauthorized claim or a 38 U.S.C 1725 (“Mill Bill”) claim, or if the patient died while in route to the facility.
7.4.6 Ambulance conveyance
VA regulations 38 CFR 17.1000-17.1008. Under this regulation, ambulances will be reimbursed at the lesser of (a) the amount the Veteran is personally liable or (b) 70 percent of the applicable Medicare Ambulance Fee Schedule.
The Medicare Ambulance Fee Schedule consists of a base rate plus mileage. There is no separate payment for items such as oxygen or other supplies, the number of attendants, providing an EKG during the trip, etc. The base rate varies by level of ambulance service provided, locality of the Medicare carrier area, and Point of Pickup (POP) zip code classification: urban, rural, or "super rural." The mileage fee varies by type of ambulance service: ground, fixed wing, or rotary wing, POP zip code classification, and loaded mileage.
Payment of ambulance transportation under 38 U.S.C. § 1725 may only be made if payment to the facility for the emergency care is authorized, or death occurred during transport.
7.4.7 Coordination with other payers
If a claim is filed for an eligible episode of care, VA must pay the whole amount according to the payment rules noted above. VA will not pay merely a deductible, copayment, or COB (coordination of benefits) amount.
VA payment constitutes payment in full. Providers cannot bill both VA and the patient or another insurer for the same encounter. If, however, VA is authorized to pay for only certain days in an inpatient stay, then the provider may bill the patient for the remaining days. Providers are not required to accept VA payment in all cases. If the provider declines VA payment then it may be able to charge the patient a greater total amount.
When possible, VA will seek reimbursement for Non-VA Medical Care payments from sources such as workers compensation payments; payments resulting from motor vehicle accidents, crimes of personal violence, or torts; other agencies when the patient is a beneficiary; and third-party insurance plans.
The Veterans’ Emergency Care Fairness Act (Public Law 111-137), signed February 1, 2010, authorizes VA as a secondary payer to third party liability insurance not related to health insurance. The Act amends 38 U.S.C. 1725 (the “Mill Bill”) by enabling VA to pay for or reimburse Veterans enrolled in VA health care for the remaining cost of emergency care if the liability insurance only covered part of the cost. Previously, VA could reimburse Veterans or pay non-VA hospitals directly only if a Veteran has no other health insurance. VA may reconsider and provide retroactive reimbursements for emergency treatment that was provided prior to the date of enactment (July 19, 2001), if documentation sufficiently demonstrates the original denial was because the Veteran received partial third party payment.
_____________________________________________________________________________
Notes and Recommendations
- Some Non-VA Medical Care claims are rejected for untimeliness or lack of statutory authority. For these reasons, the program does not pay for 100% of care that was otherwise eligible.
______________________________________________________________________________
8. Resources
VHA Office of Community Care
(Revised March 2018)
The VHA Office of Community Care is the contact for all VA community care programs. More information about can be found on their website: https://www.va.gov/communitycare/. VA intranet users can visit https://vaww.va.gov/communitycare/ (intranet only).
References
March 2018: Due to the transition of the National Non-VA Medical Care Program Office to the VHA Office of Community Care and updates to the VINCI website, some documents may no longer be available.
1. U.S. Department of Veterans Affairs. Office of Media and Public Relations. Veterans Access, Choice, And Accountability Act of 2014: Title I: Choice Program and Health Care Collaboration [online]. Accessed October 16, 2015. Available at: http://www.va.gov/opa/choiceact/documents/Choice-Program-Fact-Sheet-Final.pdf.
2. U.S. Department of Veterans Affairs. Veterans Health Administration. Veterans’ Choice Program Eligibility Details [online]. Accessed October 16, 2015. Available at: http://www.va.gov/opa/choiceact/documents/FactSheets/Veterans_Choice_Program_Eligibility_Details_August_1_Removal.pdf..
3. U.S. Department of Veterans Affairs. Veterans Health Administration. Veterans Choice Program (VCP) Overview [online]. Updated August 26, 2015. Accessed October 16, 2015. Internal use only.
4. U.S. Department of Veterans Affairs. Veterans Health Administration. Veterans Access, Choice, and Accountability Act of 2014 (VACAA): The Choice Program and the Choice Card [presentation]. March 2015.
5. U.S. Department of Veterans Affairs. Veterans Health Administration. Working with the Veterans Health Administration: A Guide for Providers [online]. Accessed October 16, 2015. Available at: http://www.mssny.org/Documents/Enews/Aug%208%202014/VA%20ProvidersGuide.pdf
6. VIReC. U.S. Department of Veterans Affairs. VA Information Resource Center VHA Corporate Data Warehouse [webpage]. Updated September 21, 2015. Accessed October 16, 2015. Available at: http://vaww.virec.research.va.gov/CDW/Overview.htm
7. VIReC. U.S. Department of Veterans Affairs. VA Information Resource Center. VIReC Research User Guide: VHA Medical SAS® Outpatient Datasets FY2006. Edward J. Hines, Jr. VA Hospital, Hines, Ill. 2007.
8. American Society of Health-System Pharmacy (ASHP). Reimbursement for Pharmacist’s Services in a Hospital-based, Pharmacist-managed Anticoagulation Clinic. June 5, 2009. Accessed October 27, 2015.
9. VINCI. U.S. Department of Veterans Affairs. VA Informatics and Computing Resource Center (VINCI). VINCI Data Description: Fee/Purchased Care [online; VA intranet only]. Accessed October 07, 2015.
10. Smith MW, Chow A. Non-VA Medical Care (Fee Basis) Data: A Guide for Researchers. Menlo Park, CA. VA Palo Alto, Health Economics Resource Center; October 2013.
11. NNPO. U.S. Department of Veterans Affairs. Chief Business Office. National Non-VA Medical Care Program Office (NNPO). Fee Purpose of Visit (FPOV) Document [online; VA intranet only]. Accessed October 16, 2015.
12. VINCI. U.S. Department of Veterans Affairs. VA Informatics and Computing Resource Center (VINCI). VINCI Data Description: Dimension [online; VA intranet only]. Accessed October 07, 2015.
13. Data Quality Analysis Team. Linking Patient Data in the CDW Update [online; VA intranet only]. Office of Information and Analytics. Health Information Governance. Data Quality Program. Business Product Management. April 14, 2014. Accessed October 16, 2015. Available at: http://vaww.vhadataportal.med.va.gov/Resources/DataReports.aspx.
14. Data Quality Analysis Team. Identifying Veterans in the CDW [online; VA intranet only]. Office of Information and Analytics. Health Information Governance. Data Quality Program. Business Product Management. April 08, 2014. Accessed October 16, 2015. Available at: http://vaww.vhadataportal.med.va.gov/Portals/0/DataQualityProgram/Reports/Identifying_Veterans_in_CDW.pdf
15. Smith MW, Su P, Phibbs CS. Matching outpatient prosthetics order records in the VA National Prosthetics Patient Database (NPPD) to health care utilization databases. Journal of Rehabilitation Research and Development. 2010;47(8):725-37.
16. Cunningham, K. VA implements the first of several Veterans Choice Program eligibility expansions. VAntage Point. U.S. Department of Veterans Affairs. October 1, 2015. Accessed October 16, 2015. Available at: http://www.blogs.va.gov/VAntage/23201/va-implements-the-first-of-several-veterans-choice-program-eligibility-expansions/.
17. NNPO. U.S. Department of Veterans Affairs. Chief Business Office. National Non-VA Medical Care Program Office (NNPO). Non-VA Payment Methodology Matrix [online; VA intranet only]. Accessed October 16, 2015.
[1] The Health Care Financing Administration (HCFA) was renamed the Centers for Medicare and Medicaid Services.
AcknowledgementsThis research was supported by the Health Systems Research Service, U.S. Department of Veterans Affairs (ECN 99017-1). We gratefully acknowledge comments and contributions from Sharon Dally, Susan Schmitt and Paul Barnett. Mark Smith and Adam Chow were the authors of the original HERC guidebook, upon which this document builds. We are grateful for their cogent work.
Last Updated Date: 2019-04-03














